Venous Malformation Case Report
Yousif I Eltohami, Nour E Alim and Amal H Abuaffan
DOI10.4172/2471-9781.100016
Yousif I Eltohami and Amal H Abuaffan*
Faculty of Dentistry, University of Khartoum, Sudan
- *Corresponding Author:
- Abuaffan AH
Faculty of dentistry
University of Khartoum, Sudan
Tel: +249 91 778 8622
E-mail: amalabuaffan@yahoo.com
Received date: November 21, 2016; Accepted date: November 29, 2017; Published date: November 30, 2017
Citation: Eltohami YI, Abuaffan AH. Venous Malformation Case Report. J Hosp Med Manage. 2016, 2:2.
Abstract
Venous malformations in the maxillofacial region are difficult to manage. Sclerosing agents like hypertonic saline, ethanol, sodium tetradecylsulfate, polidocanol, are recommended for the treatment. The current case reports a venous malformation in the tongue treated with hot saline, a safe, effective and inexpensive modality for treatment of vascular malformations. Proper diagnosis and case selection are a must for the management to minimize possible risks and complications. The findings in this case suggest that sclerotherapy with hot saline is a safe and effective method for treatment.
Keywords
Venous malformation; Tongue; Hot saline; Congenital
Introduction
Vascular malformations accounting for approximately 7% of all benign tumors, the majority was developing in the head and neck region [1]. Vascular malformations are subdivided into high flow and low flow malformations, the later involve the venous malformations. The overall incidence of venous malformations is about one in 10000. These lesions commonly occur in the head and neck with a predilection for the oral cavity, airway and muscle groups. These lesions will continue to grow throughout the patient's life [2]. Venous malformations (VMs) morphologically and histologically similar to veins. They are classified as superficial or deep and as localized, multicentric or diffuse. The skin or mucosa that covers such malformations varies in color according to the depth and degree of ectasia of the lesion. The most superficial ones are purple in color, whereas the deeper ones appear more bluish or greenish or may not even be visible [3]. Generally, vascular malformations in the maxillofacial region represent an aesthetic problem. Nevertheless, tongue lesions in the majority of cases can cause clinical problems like spontaneous hemorrhage from the mouth; progressive asymmetric growth of the tongue (macroglossia) can be also observed [1].
Case Report
• A 28 years old Sudanese female came to oral and maxillofacial surgery clinic complaining from painless soft swelling in the right side of the tongue presented at birth and increasing gradually in size coinciding with her age.
• No significant medical or social history.
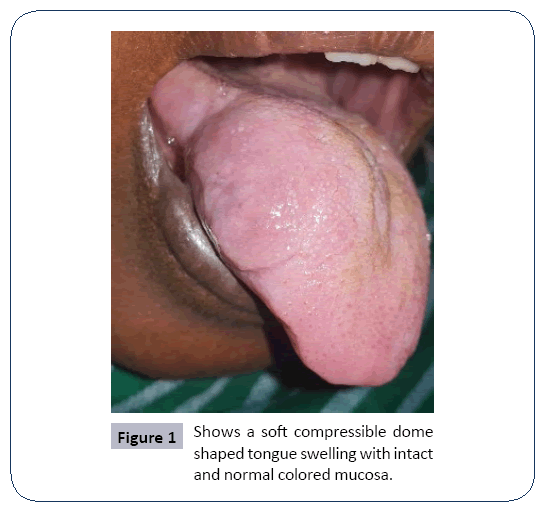
• Clinical examinations show a non-tender warm soft compressible dome shaped tongue swelling with intact and normal colored mucosa. No apparent discharge and thrills or bruits (Figure 1).
• On aspiration biopsy, there is a blood.
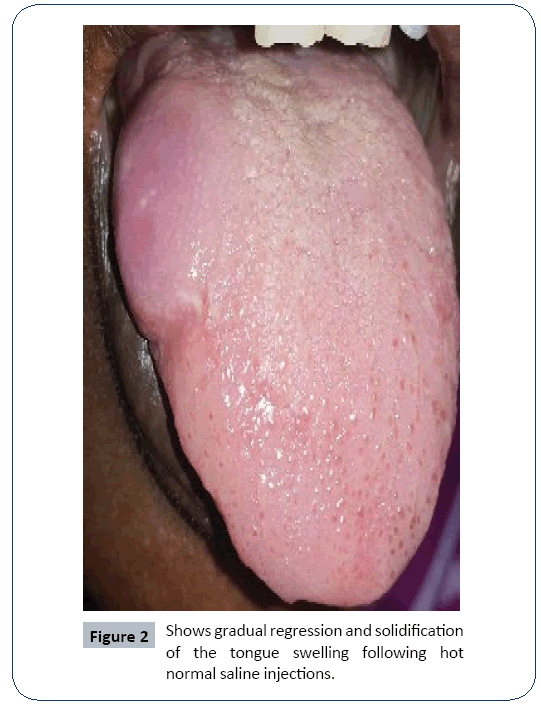
• Patient was treated by regular injections of hot normal saline as sclerotic agent and showed gradual regression and solidification of the swelling (Figure 2).
Discussion
Venous malformations are common vascular malformations, in the head and neck region it accounts 40% approximately [4]. Present at birth and slowly growing during childhood, and may enlarge during trauma, puberty, and pregnancy; due to the hormonal changes and composed of an abnormal collection of veins, which are thin-walled, sponge-like channels of variable size, lacking in smooth muscle. In general it bluish compressible mass and tend to slowly expand with time [5-7]. Vascular malformations can be classified as: congenital: occurring as a result of lack of differentiation of arteries, capillaries, and veins during vascular development, and acquired, associated with previous history of injury/trauma.
In the oral cavity, it can present at any site, but most commonly on anterior two-thirds of tongue, leading to macroglossia and difficulty in mastication, speech, and deglutition. Other sites that may be involved are palate, gingiva, and buccal mucosa [8]. The diagnosis of vascular malformations is based on the patient’s medical history and a physical examination [9]. Vascular low flow lesions have progressive increase with age, trauma, and after partial resection. We believe that our case corresponds to vascular low flow malformation due to their bluish-purple aspect, consistence, and the absence of vascular pulsation [10]. Venous malformations can be managed by observation, irradiation, electro coagulation, cry therapy, low-dose aspirin, sclera therapy, surgical excision, or combinations [11-13]. Sclera therapy is commonly the preferred treatment method for venous malformations [14]. Various agents for sclera therapy; OK-432, ethanol, bleomycin, doxycycline, sodium tetradecyl sulfate, and hypertonic saline, alone or in combination [15]. The best-known sclerosant in the United States was hypertonic saline sodium chloride 23.4%. It was nonspecific in cellular destruction it causes dehydration to endothelial cells and red blood cells. Patients preferred “saline injections,” which has become synonymous with injection sclera therapy. The drug was readily available, lacks allergenicity, and was inexpensive [16,17]. Boiling water and warm hypertonic saline solutions have been variously used by Obuekwe et al. [18] and Oji et al. [19] in treating venous malformations. They act by releasing heat energy that destroys the anomalous vascular tissues. More than boiling water, boiling saline retains heat energy which can adversely affect the vascular endothelial tissues which lead to necrosis and obliteration of the vessels’ Lumina, which regularly promotes coagulation of blood and death of the vessels [20]. The potential complications of sclera therapy include mucosal ulcerations, swelling, infection, transient nerve palsy, blood loss, and anaphylaxis [15,16]. In the current case study, using the hypertonic hot saline was very effective and a safe method as the lesion responds considerably and shrink in size without complications.
Conclusion
Venous malformations of the tongue may associated with several complications, proper diagnosis and case selection are a must to for the management and conservative treatment is preferred, in this case sclera therapy with hot saline is a safe and effective method for treating venous malformations in the oral region.
References
- Cappabianca S, Del Vecchio W, Giudice A, Colella G (2006) Vascular malformations of the tongue: MRI findings on three cases. Dentomaxillofac Radiol 35: 205-208.
- Buckmiller LM, Richter GT, Suen JY (2010) Diagnosis and management of hemangiomas and vascular rmalformations of the head and neck. Oral Dis 16: 405-418.
- Redondo P (2007) Vascular malformations (I). Concepts, classification, pathogenesis and clinical features. Actas Dermosifilogr 98: 141-158.
- Scolozzi P, Laurent F, Lombardi T, Richter M (2003) Intraoral venous malformation presenting with multiple phleboliths. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 96: 197-200.
- Garzon MC, Huang JT, Enjolras O, Frieden IJ (2007) Vascular malformations: part I. J Am Acad Dermatol 56: 353-370.
- Rosbe KW, Hess CP, Dowd CF, Frieden IJ (2010) Masseteric venous malformations: diagnosis, treatment, and outcomes. Otolaryngol Head Neck Surg 143: 779-783.
- Tan ST, Bialostocki A, Brasch H, Fitzjohn T (2004) Venous malformation of the orbit. J Oral Maxillofac Surg 62: 1308-1311.
- Shetty DC, Urs AB, Rai HC, Ahuja N, Manchanda A (2010) Case series on vascular malformation and their review with regard to terminology and categorization. Contemp Clin Dent 1: 259-262.
- Mulliken JB, Glowacki J (1982) Hemangiomas and vascular malformations in infants and children, A classification based on endothelial characteristics. Plast Reconstr Surg 69: 412-422.
- Redondo P (2004) [Classification of vascular anomalies (tumours and malformations). Clinical characteristics and natural history]. An Sist Sanit Navar 27: 9-25.
- Bowman J, Johnson J, McKusick M, Gloviczki P, Driscoll D (2013) Outcomes of sclerotherapy and embolization for arteriovenous and venous malformations. Semin Vasc Surg 26: 48-54.
- Nguyen JT, Koerper MA, Hess CP, Dowd CF, Hoffman WY, et al. (2014) Aspirin therapy in venous malformation: a retrospective cohort study of benefits, side effects, and patient experiences. Pediatr Dermatol 31: 556-560.
- Rubin BA, Brunswick A, Riina H, Kondziolka D (2014) Advances in radiosurgery for arteriovenous malformations of the brain. Neurosurgery 74:S50-S59.
- Lee B, Do Y, Byun H, Choo I, Kim D, et al. (2003) Advanced management of venous malformation with ethanol sclerotherapy: mid-term results. J Vasc Surg 37: 533-538.
- Richter GT, Friedman AB (2012) Hemangiomas and vascular malformations: current theory and management. Int J Pediatr 2012: 1-10.
- Wiegand S, Eivazi B, Zimmermann AP, Sesterhenn AM, Werner JA (2011) Sclerotherapy of lymphangiomas of the head and neck. Head Neck 33: 1649-1655.
- Dietzek CL (2007) Sclerotherapy: Introduction to Solutions and Techniques. Perspect Vasc Surg Endovasc Ther 19: 317-324.
- Obuekwe ON, Ojo MA, Akpata O, Saheb BD (2002) Haemangioma of the maxillofacial region in Benin City, Nigeria. Ann Biomed Sci 1: 18-22.
- Oji C, Chukwuneke FN, Mgbor N (2005) Tobacco-Pouch suture technique for the treatment of vascular lesions of the lip in Enugu, Nigeria. Br J Oral Maxillofac Surg 44: 245-247.
- Ketan RB, Sunny S, Shahid MN (2006) Histrory of bipolar coagulation. Neurrosurg Rev 29: 93-96.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences